Nourishing the Flower
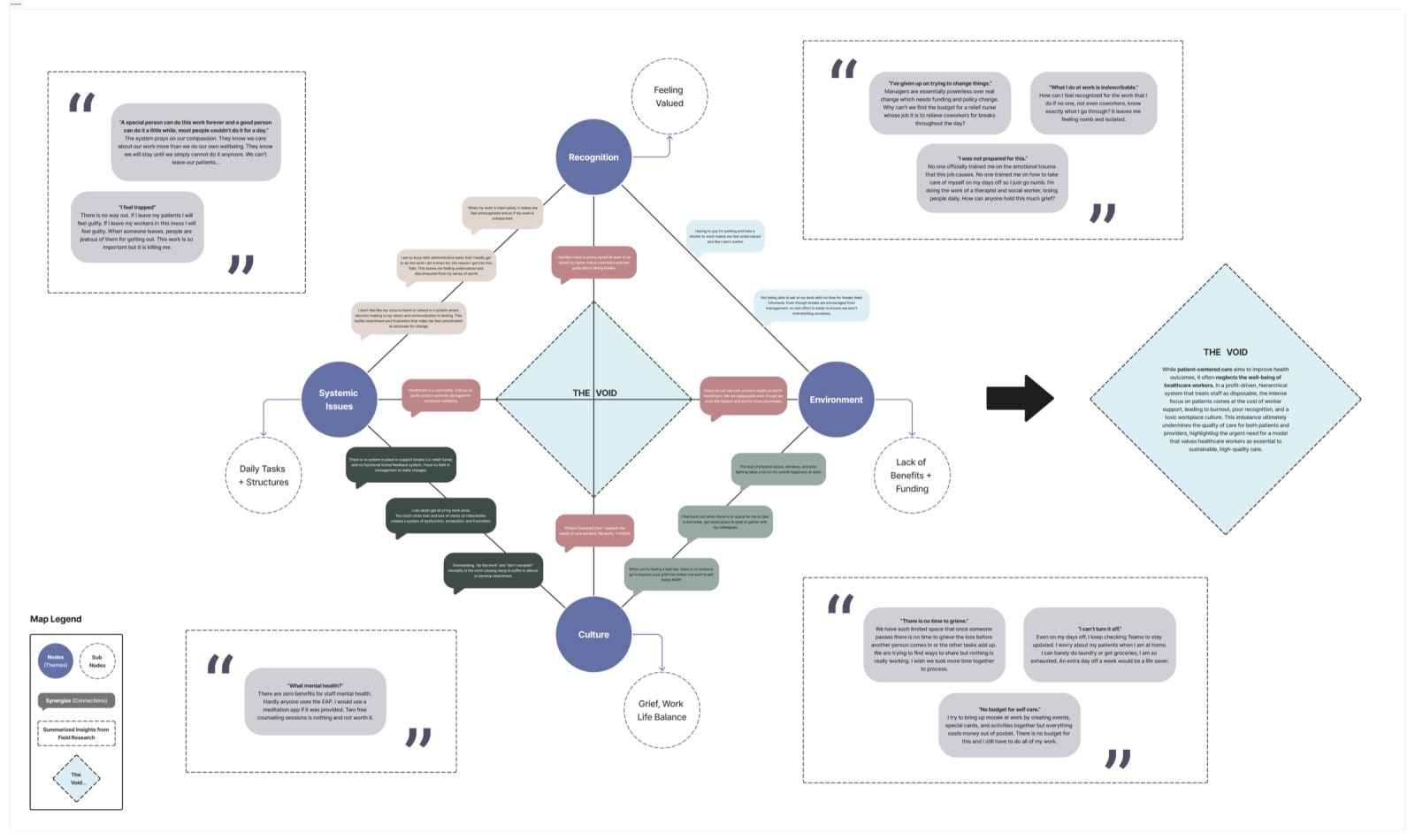
Using the anatomy of a flower as a metaphor for workplace health, participants mapped their experiences onto two worksheets—one flourishing, one wilting. The exercise surfaced what sustains people alongside what quietly erodes them. The session ended with the group voting on what resonated most.
“Positive atmosphere, positive energy. Team player. Support one another.”